The Goal of Your Hip Replacement
Our primary goal with your hip replacement is to deliver a procedure so accurate and optimally balanced that once you’ve recovered, you can’t tell you ever had surgery. This is considered a “forgotten joint” and is what every surgeon strives to achieve for their patients.
Traditional hip replacement offers a cookie-cutter approach to surgery. Alignment is based on the surgeon’s calculations during surgery. With Kinomatic custom surgical planning, your surgeon will plan out every detail of your surgery with unmatched precision to create a custom surgical template. Kinomatic surgical planning removes the guesswork, and helps your surgeon achieve the best possible outcome, a forgotten hip.
What Makes a Custom Hip Replacement Unique from Traditional Surgery
Taking the Guesswork out of Surgery
Custom Surgery allows your surgeon to know everything about your anatomy and your surgery in advance resulting in more accurate and efficient procedures.
Personalized to Best Fit your Unique Anatomy
We take countless measurements of your entire lower anatomy. This allows us to personally plan your knee replacement that’s going to feel like a natural joint.
Optimized Surgery for an Optimized Recovery
Because Kinomatic procedures involve less intraoperative guesswork, patients will typically experience less pain and get back to normal activity more quickly.
Hip Replacement by the Numbers
450K
Hip replacements are performed annually in the U.S.
635K
Projected hip replacements by the year 2030 in the U.S.
95%
Hip replacement patients experience pain relief and improved function.
65 Years
Is the average age of a hip replacement patient.
Symptoms of Hip Pain
Your hip makes popping or crunching sounds when in motion
Hip is red or warmer than the surrounding tissue
Knee feels weak or unstable
Stiffness or sensation of tightness in the hip joint
Learn More About Hip Replacements

What are the Common Causes of Hip Pain?
Symptoms of a damaged hip joint vary, based on the underlying hip condition. The symptoms may include:
- Stiff hip
- Hip is red or warmer than the surrounding tissue
- Hip feels weak or unstable
- Your hip makes popping or crunching sounds when in motion
Other Causes of Hip Pain
Chronic hip pain is commonly caused by arthritis. Arthritis is a term used to describe pain and inflammation in the joints. While there are many types of arthritis, the three most common types that lead to pain and loss of mobility are:
Osteoarthritis
According to the Centers for Disease Control and Prevention (CDC), osteoarthritis (OA) is the most common type of arthritis. Osteoarthritis is an age-related form of arthritis that causes joint pain and stiffness. As we age, the cartilage that cushions our joints begins to wear away, eventually leading to painful bone-on-bone contact. This type of arthritis is more common in people over 50 years of age, although it has been seen in younger patients. Osteoarthritis is the most chronic condition of the joints which affects approximately 27 million Americans.
Symptoms often develop slowly and tend to worsen over time. Typical signs and symptoms include; pain in your joints with movement, tenderness, stiffness, loss of flexibility limiting range of motion, and bone spurs (extra bits of bone which feel hard and can form around the joint). Common risk factors of osteoarthritis include: increasing age, obesity, previous injury, joint overuse, weak muscles, and genetics. There is no proven treatment for osteoarthritis. The most common way to help alleviate osteoarthritis is by physical measures, drug therapy, and surgery.
Osteoarthritis was once believed to be just “wear and tear” on the joint as a natural part of aging. The condition is now viewed as a disease that attacks the joints in the body. Several issues can contribute to the development of osteoarthritis in the hip joints, including:
Genetic Predisposition
Some genetic factors come into play, and it is believed that some people have a defect in the genetic code that directs collagen production in the body. Other patients may have inherited a minor flaw in how the hip joints fit together that leads to faster wearing of the cartilage.
Weight
When a person carries excess weight, it naturally places more stress on the weight-bearing joint at the hip. This causes the cushioning cartilage to wear away more quickly. It is believed by some researchers that the presence of excess fat in the body leads to the production of inflammatory chemicals that may damage the joint.
Injury, Excessive Hip Use
Some people have performed repetitive motions at work, in athletic pursuits, running, or other activity that eventually affects the function of the hip joint. Types of jobs that involve a great deal of time standing, lifting, or other similar activity can wear away the joint more rapidly. Injuries to joints such as damage from a fall, car accident, or other event can lead to a fracture which eventually leads to developing osteoarthritis.
Rheumatoid Arthritis (RA)
Rheumatoid Arthritis (RA) is a disease that causes the synovial membrane around the hip to become inflamed and thickened. This autoimmune disorder can damage the cartilage over time, causing cartilage loss, joint pain, and stiffness.
Post-Traumatic Arthritis
Post-traumatic Arthritis is the result of a major injury to the hip. Bone fractures, ligament tears, and resulting damage to the cartilage over time will result in arthritis of the hip or knee.
Avascular Necrosis
Avascular necrosis is a condition where the blood supply to the bones is disrupted, leading to bone cell death and damage to the bone structure. This can cause joint pain, stiffness, and reduced mobility. In the case of the hip joint, vascular necrosis can affect the femoral head, the rounded top of the thigh bone that fits into the hip socket.
Over time, the damage caused by vascular necrosis can progress to the point where the femoral head collapses or becomes deformed. This can cause further pain and difficulty with movement and may lead to the need for total hip replacement surgery. Similar to a total hip replacement from rheumatoid or osteoarthritis, the damaged bone will be resected and replaced with an artificial joint. A metal stem is used to replicate the femoral neck and a ceramic ball for the femoral head that will articulate with a metal cup and polyethylene liner that replaces the acetabulum (hip socket).
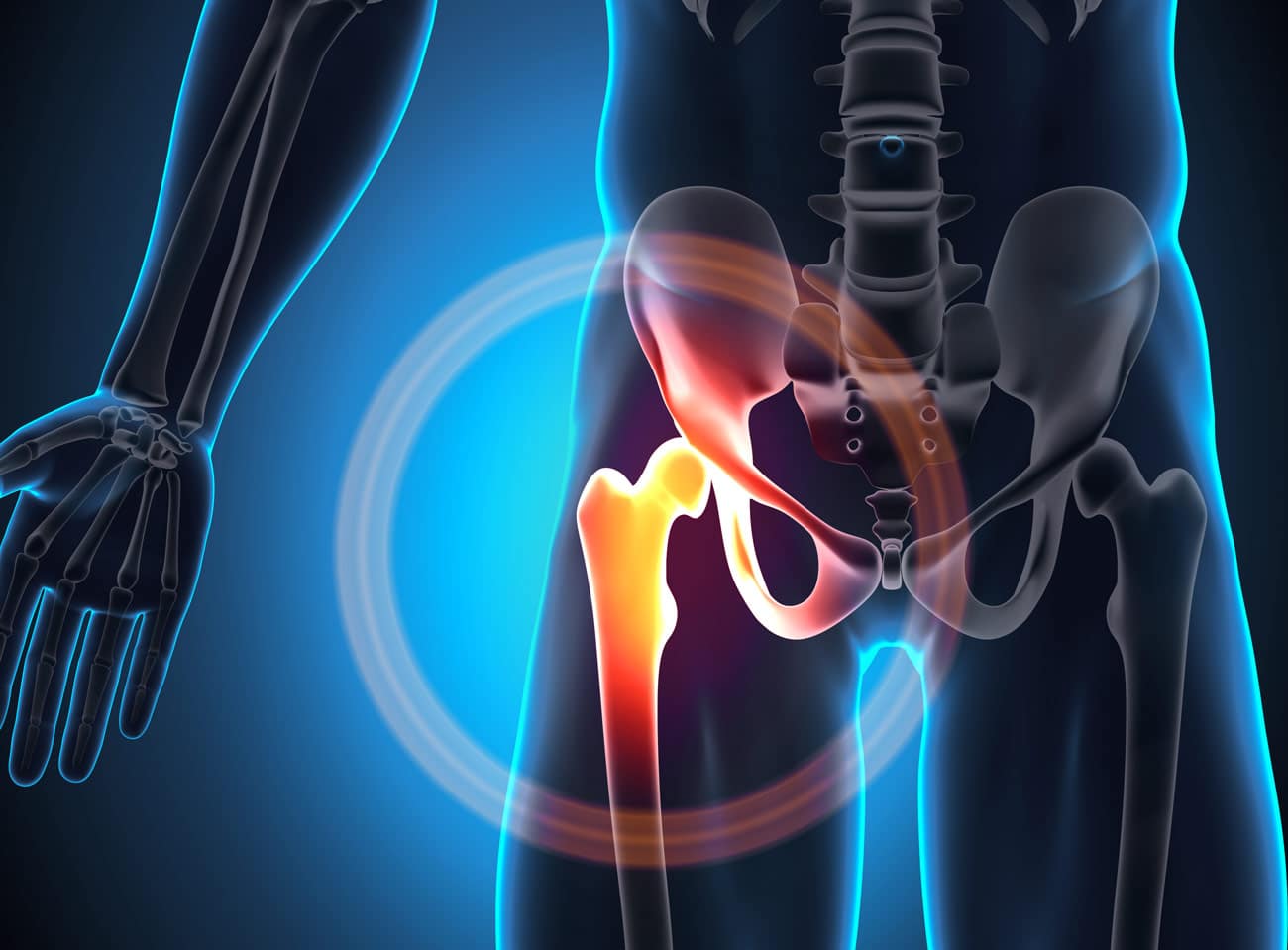
Alignment and Kinematics of the Hip
Proper alignment involves the pelvis being level, and the femur (thigh bone) being properly positioned in the acetabulum (hip socket). In cases of hip osteoarthritis, this alignment can be compromised, resulting in abnormal forces on the joint during walking. This can lead to increased pain, further joint damage, and reduced mobility.
During walking, the hip undergoes three different types of motion, including flexion, extension, and abduction. Flexion is the movement of the thigh bone towards the front of the body, extension is the movement of the thigh bone towards the back of the body, and abduction is the movement of the thigh bone away from the midline of the body. These movements are made possible by the complex anatomy of the hip joint, which consists of the femoral head, the acetabulum, the labrum, and the surrounding muscles, ligaments, and tendons. The proper function of the hip joint is essential for a smooth and efficient gait, and any abnormalities or injuries can significantly impact an individual’s ability to walk. If these functions are chronically altered by rheumatoid or osteoarthritis, a total joint replacement may be necessary.

Hip Replacement (Total Hip Arthroplasty)
Hip replacement, also called total hip arthroplasty, is a surgical procedure in which the worn out or damaged surfaces of the hip joint are removed and replaced with new parts. The hip is a ball in socket joint. The articular cartilage that lines the head of the femur will wear out over time causing extreme pain and difficulty in performing daily activities. Once the cartilage has worn out the head of the femur starts to rub against the acetabulum the recommended treatment is to replace the ball and socket joint with a synthetic joint made of titanium and ceramic. Aligning the ball and socket with your natural biomechanical alignment is critical to achieving a natural feeling hip. Kinomatic VR allows your surgeon to perfectly align your hip to achieve a hip that feels so natural you’ll forget you ever had surgery.
Hip Replacement Surgical Approaches
Surgical techniques for total hip replacement have evolved over the years, with advancements in technology and improvements in surgical instruments and implants. The two main approaches for total hip replacement are the posterior and the anterior approach. In the posterior approach, the surgeon makes an incision at the back of the hip joint and detaches the muscles to access the hip joint. In the anterior approach, the surgeon makes an incision at the front of the hip joint and works between the muscles, avoiding muscle detachment. This approach has gained popularity in recent years due to potentially faster recovery time and lower dislocation rates. Both have pros and cons and are worth discussing with a surgeon before a total hip replacement.
The Option of Personalized Hip Replacement
Total hip replacements (THR) are one of the most successful surgical procedures, providing pain relief and improved mobility to patients with hip arthritis or other hip joint pathologies. According to a study by the National Joint Registry, the 10-year survival rate of THR is 92%, while the 20-year survival rate is 82%. However, there are still cases of implant failures, dislocations, and infections. Personalized hip replacements have emerged as a potential solution to improve the long-term outcomes of hip replacements.
Kinomatic utilizes CT scans to create a 3D image of the patient’s bones. Various measurements are made on the bones with data that surgeons traditionally do not have access to with a routine X-ray. For example, leg length measurements can be used to find anatomical discrepancies that should be factored in when surgically altering the hip joint. Preoperative planning is personally tailored to the patient with custom sizing and placement of a femoral stem, femoral head, and acetabular cup. This allows for further accuracy and customization with a Kinomatic preoperative plan.
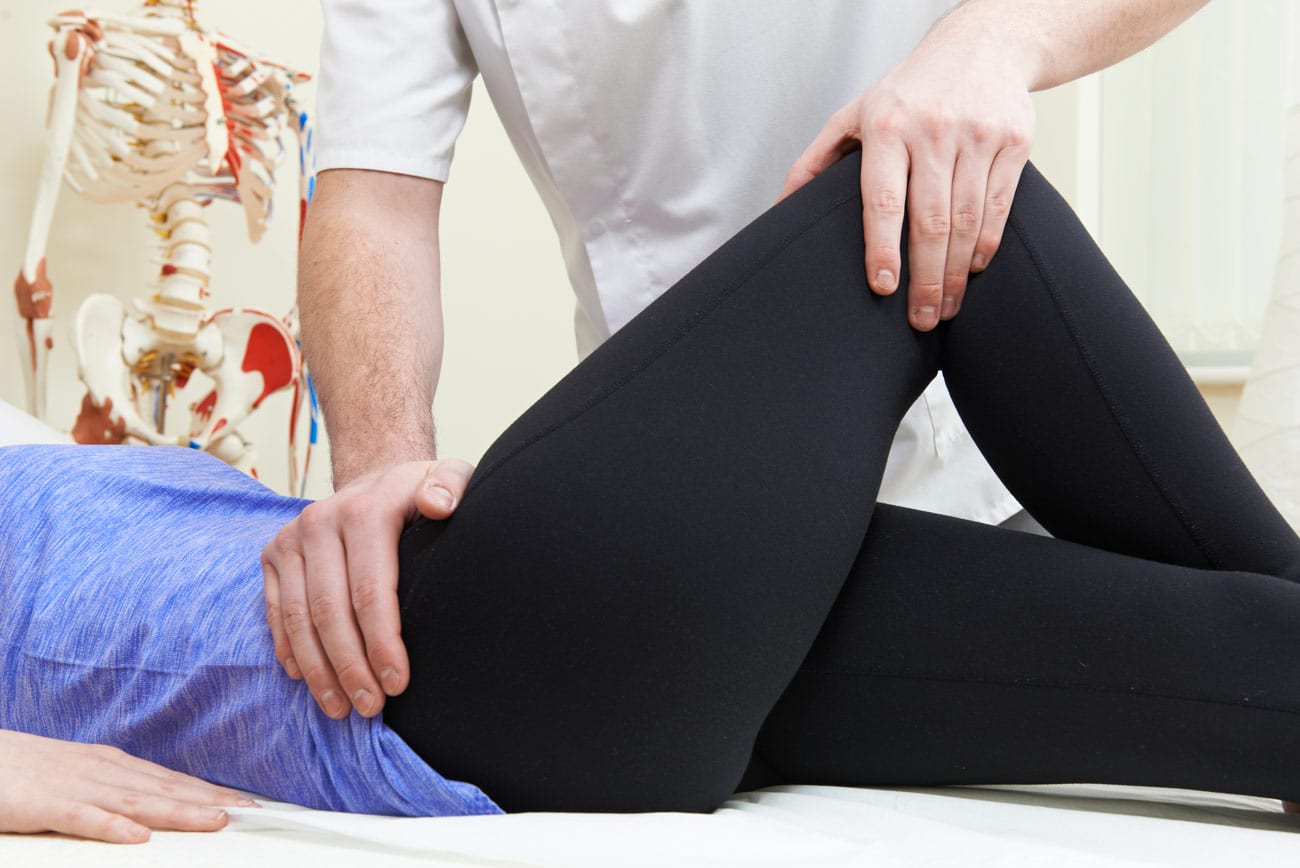
Post-Op Hip Replacement & Physical Therapy
Physical therapy is an integral part of postoperative care after total hip replacement (THR). Physical therapy typically begins immediately after surgery and continues for several weeks to months, depending on the patient’s progress. The goals of physical therapy after THR include improving range of motion, strength, and balance, reducing pain and swelling, and facilitating a safe return to daily activities. Physical therapy programs may include exercises to improve hip flexion, extension, abduction, and adduction, as well as exercises to strengthen the hip and surrounding muscles. Other interventions, such as gait training, balance exercises, and modalities like ice or heat therapy, may also be utilized. Several studies have reported that physical therapy after THR can lead to improved functional outcomes, reduced pain and stiffness, and increased patient satisfaction.
Kinomatic implements a personalized physical therapy plan post THR through OneStep to take the patient from a custom preop plan all the way through postop for an ideal functional outcome.
Functional Outcomes of Hip Replacement
Total hip replacement has been shown to provide significant improvements in quality of life and functional outcomes for patients with hip arthritis or other hip joint pathologies. Studies have demonstrated improved pain relief, increased range of motion, and better mobility following total hip replacement. In addition, total hip replacement has been associated with improved psychological well-being and social functioning. Patient satisfaction rates are generally high, with one study in the Journal of Arthroplasty reporting a 95% satisfaction rate among patients who underwent total hip replacement. However, there are some factors that may affect the outcomes of total hip replacement, including age, preoperative physical function, and postoperative physical therapy. A preoperative plan is the first step to optimal satisfaction and accuracy in surgery.